Key messages
- The most common types of diseases that affect the gums are gingivitis and periodontitis.
- Gingivitis is the mildest and most common type.
- When gingivitis is not controlled the inflammation progresses to periodontitis.
- If periodontitis is not treated, you can lose some or all of your teeth.
There are a range of diseases that affect the gums. These are called periodontal diseases. The most common types of periodontal disease are gingivitis and periodontitis.
Gingivitis
Gingivitis is the mildest and most common type of periodontal disease.
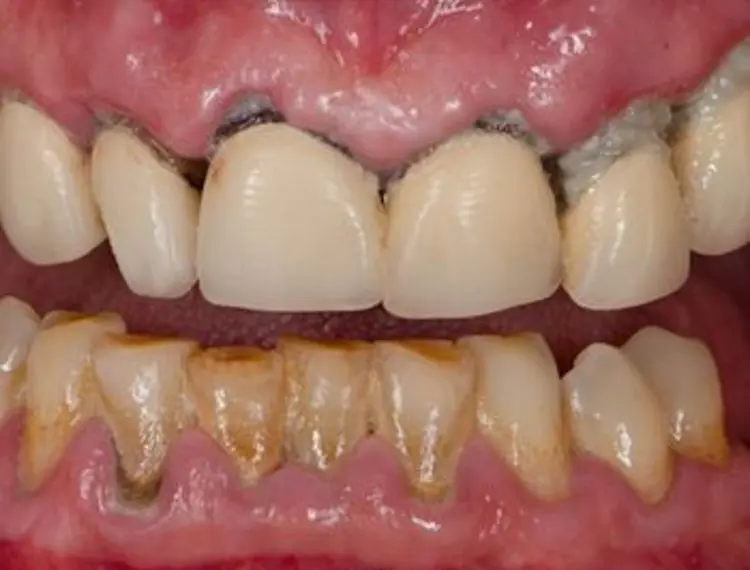
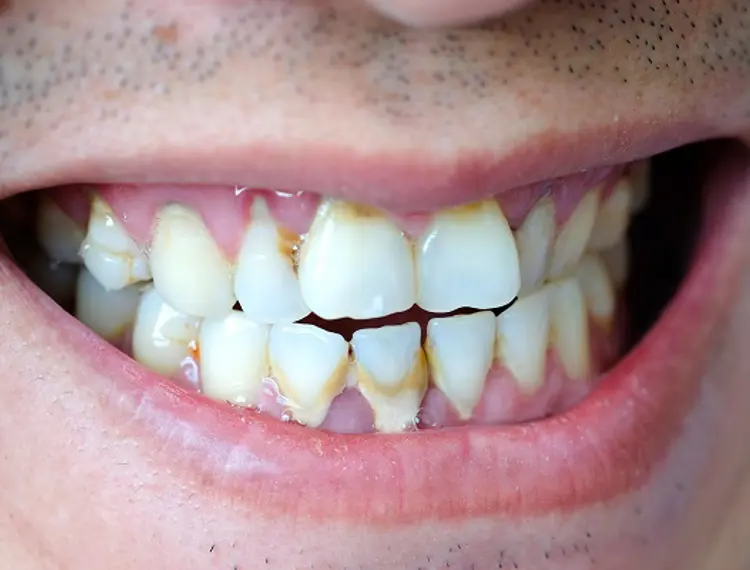
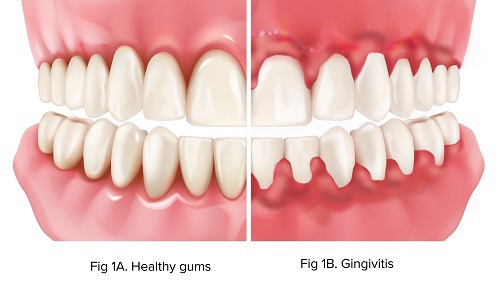
Poor oral hygiene causes a build-up of bacteria where the teeth and gums meet. This causes the gums to become inflamed. (Figure 1B) Common signs are redness, swelling, and bleeding. It can sometimes cause discomfort. This can lead to more serious problems.
You can treat gingivitis with professional teeth cleaning and taking good care of your teeth at home. It's important to visit a dentist if your gums bleed when cleaning your teeth or eating. Your dentist will check the cause for the bleeding.
Periodontitis
When gingivitis is not controlled the inflammation progresses to periodontitis. Periodontitis is a common chronic disease that affects around 1 in 4 adults.
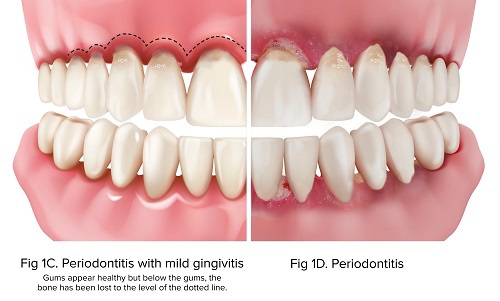
Periodontitis is caused by damaging bacteria that can cause damage to the gums and bone that support the teeth. (Figure 1C-Figure 1D). This causes pockets of space under the gums around the teeth.
Factors that can increase your risk of periodontitis include:
- poor oral hygiene
- a family history of periodontitis
- medical conditions, such as diabetes
- harmful habits, such as smoking.
Periodontitis does not usually cause pain. Common signs of the disease include:
- gums pull back making the teeth look longer
- loose teeth
- teeth moving.
If periodontitis is not treated, you can lose some or all of your teeth. Treatment by a dental practitioner is needed to stop the disease from getting worse.

This content was created in collaboration with the
Australian & New Zealand Academy of Periodontitists (ANZAP).